
|Takeaways|
■ LDL-C is type of lipoproteins that leads to atherosclerosis.
■ To reduce LDL-C is the primary target for cardiovascular risk control.
■ Lifestyle improvement and medication therapy such as statin are the main means to lower lipid level in blood.
■ To emphasize the concept of lipid management is to ensure vascular health.
Mr. Li, a 42-year-old man with a slight build, had a sudden heart attack and a stent was placed. In the post-operative examination, he was found to have abnormal lipids reading (LDL-C: 4.68 mmol/L), and was required by his doctor to control his blood lipids level and to have the anticoagulation treatment. Mr. Li was rather confused. Why is lipid control necessary for the treatment of heart attack? How to lower lipids and what tests are needed? How low should the level be maintained at?
Q1. What are blood lipids?
Lipids is a general term for the lipids (fat) contained in blood plasma, including total cholesterol (free cholesterol and cholesteryl esters), triglycerides (TG), free fatty acids (FFA), phospholipids, and glycolipids.
There are two sources of lipids in the blood. Exogenous lipids are ingested from food and endogenous lipids are synthesized by liver cells, adipocytes and other tissue cells. Blood lipids tend to fluctuate widely as it’s often influenced by diet, age, gender, occupation and metabolism.
Blood lipids are insoluble in water and usually bind to apolipoproteins to form lipoproteins before transported and metabolized in the blood. The density, size, surface charge, and physiological function of lipoprotein particles differ because of the different types and content of lipids and apolipoproteins contained. Clinically, there are five types of lipoproteins, including celiac, very low-density lipoprotein (VLDL), low-density lipoprotein (LDL), intermediate-density lipoprotein (IDL), and high-density lipoprotein (HDL), classified by their density.

Q2. What are the functions of each of the five lipoproteins?
Celiac particles are mainly responsible for transporting exogenous triglycerides and cholesterol; VLDLs are mainly responsible for transporting endogenous triglycerides; LDLs are mainly responsible for transporting endogenous cholesterol; HDLs are mainly responsible for reverse transporting cholesterol, which is produced by extrahepatic tissue cells and transported to the liver through blood circulation to be metabolized by the liver and excreted as bile acids.
Q3. Are the lipids transported by lipoproteins required by the body?
Lipids are indispensable for human life activities. For example, triglycerides provide energy to the body. Cholesterol, phospholipids and glycolipids are important components of biological membranes, involved in cell recognition and signal transduction, and are precursors of many biologically active substances. Fatty acids are metabolized to produce fatty acid derivatives which also have important physiological functions.
Q4. Why do we need to control lipids when they are so important to our body?
It is true that lipids are essential to our body's life activities, but high level of lipids in the blood can cause damage to the body (especially blood vessels). For people with high risk of cardiovascular disease, even normal level of lipids would do so.
Two major chronic diseases are threatening our health: malignant tumors and cardiovascular diseases. According to the World Health Organization, cardiovascular disease is the leading cause of death of human. Therefore, it is necessary to pay attention to the cardiovascular health.
There are many factors affecting cardiovascular health, such as age, gender, smoking, hypertension, diabetes, dyslipidemia, and family history of cardiovascular diseases.
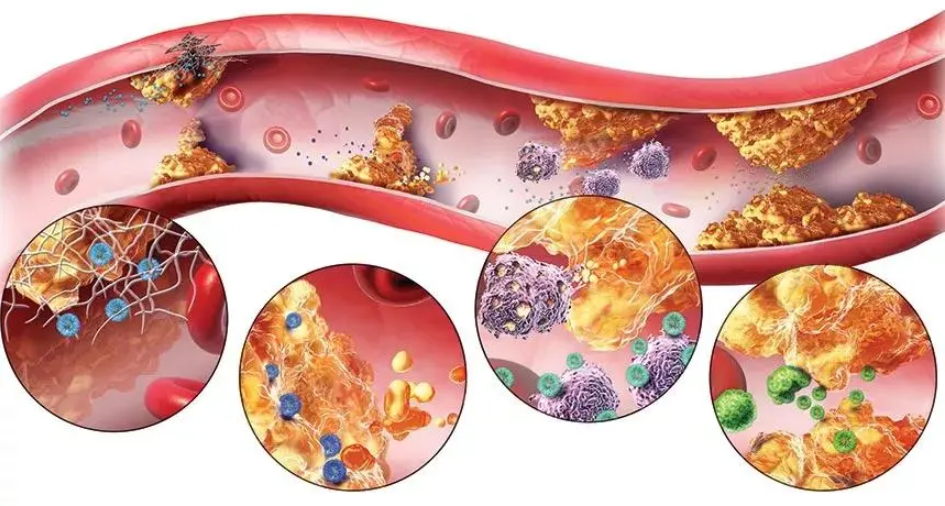
Numerous randomized clinical studies have confirmed that elevated low-density lipoprotein cholesterol (LDL-C) is a key factor in the formation of atherosclerosis and that lowering LDL-C levels significantly reduces the risk of atherosclerotic cardiovascular disease (ASCVD).
Q5. What tests are needed for lipid screening?
Regular lipid screening is an important measure in the prevention and treatment of dyslipidemia and cardiovascular diseases. It is not only used to distinguish whether the blood lipids are normal or not, but also to predict and assess the risk of cardiovascular disease in the population and to guide intervention treatment.
Lipid test generally include four basic items: total cholesterol, triglycerides, LDL-C, and HDL-C.
Other items of increasing interest:
Lipoprotein A (Lp(a)): its increase is commonly seen in ASCVD, acute heart attack, diabetes and other diseases. A lower level is better!
Apolipoprotein A (ApoA): It is the main component of HDL-C. A higher level is better!
Apolipoprotein B (ApoB): Concurrent measurement with LDL-C is good for clinical judgment. A lower level is better!
Q6. How often should blood lipids be measured? Which groups of people should be focused on?
To detect lipid abnormalities in a timely manner, it is recommended that
(1) Adults aged 20-40 should have their blood lipids measured at least once every 5 years.
(2) Men aged 40 and above and postmenopausal women should have their blood lipids tested annually.
(3) Patients with atherosclerotic cardiovascular disease and those with high cardiovascular risk should have their lipids measured every 3-6 months.
(4) Patients hospitalized for atherosclerotic cardiovascular disease should have their lipids measured at the time of admission or within 24 hours of admission.
People with following conditions should focus on their lipids level.
■ A history of ASCVD
■ High prevalence of ASCVD such as hypertension, diabetes, obesity and smoking
■ A family history of early-onset cardiovascular disease
■ Familial hyperlipidemia
■ Yellow tumors of the skin or tendons and thickened Achilles tendons
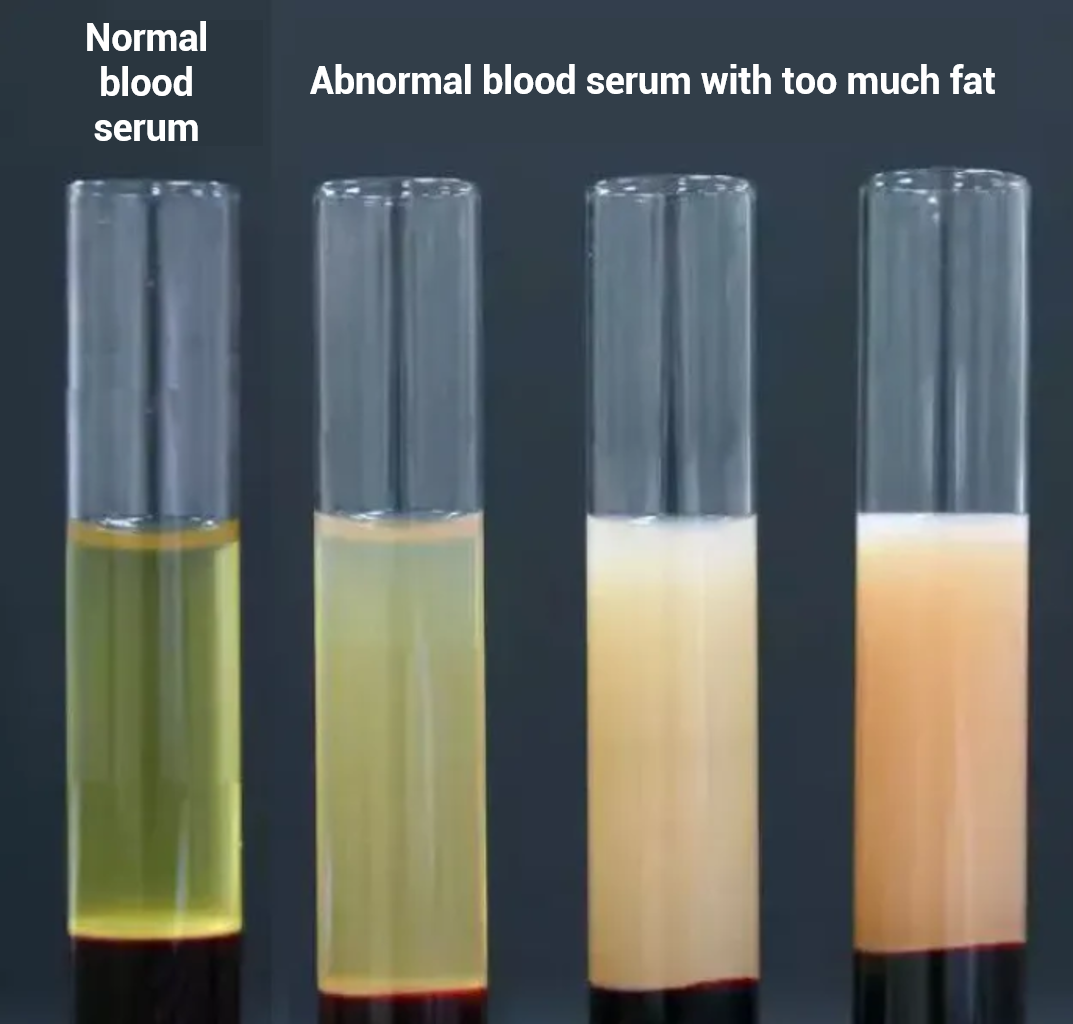
Q7. There are different reference ranges for LDL-C on the test report. How to read them?
The reference range of LDL-C is based on the values measured in the majority of the healthy population. But for every individual, it is more helpful if specific LDL-C control targets based on the risk level for cardiovascular accidents could be set.
The LDL-C/non-HDL-C reference range for people with different risks vary considerably (see table below). If you are at low/intermediate risk of cardiovascular accidents, LDL-C below 3.4 mmol/L is fine; however, if you are at very high risk, it is recommended that lipids should be monitored closely and kept below 1.8 mmol/L.

Q8. How to determine the risk of cardiovascular accident?
Patients with a clinical diagnosis of ASCVD (including acute coronary syndrome, stable coronary artery disease, post-hemodynamic reconstruction, ischemic cardiomyopathy, ischemic stroke, transient ischemic attack, peripheral atherosclerotic disease, etc.) are considered to be at very high risk of cardiovascular accident.
Those who meet one of the following conditions are classified into high-risk groups.
(1) LDL-C ≥ 4.9 mmol/L;
(2) Patients with diabetes and age ≥ 40 years and 1.8 mmol/L ≤ LDL-C < 4.9 mmol/L
If neither of the above conditions are present, the overall risk of developing ASCVD in the next 10 years can be assessed and stratified by clinicians, also taking weight, smoking, hypertension and lipids level into account.
Q9. How to control blood lipids?
Lifestyle change: There is a close relationship between dyslipidemia and lifestyle. Regardless of whether one chooses pharmacological lipid-regulating therapy, lifestyle change is the preferred option for lipid control. A good lifestyle includes controlling dietary cholesterol intake, increasing physical activity, maintaining ideal body weight, and staying away from risk factors such as tobacco.
Drug intervention therapy: Timely drug intervention is also an important method to lower lipids level. At present, the lipid-regulating drugs commonly used in clinical practice in China mainly include statins, fibrates, niacin and cholesterol absorption inhibitors. Among them, statins are most widely used in clinical practice. Statins can regulate lipids level by lowering LDL-C levels and reducing cholesterol synthesis; at the same time, they can improve vascular endothelial function, work as an antioxidant and anti-inflammatory, inhibit platelet aggregation and antithrombotic, prevent atherosclerosis formation and stabilize or reduce atherosclerotic plaques. In case patients have drug intolerance or nonstandard cholesterol level or severe mixed hyperlipidemia, the combined application of lipid-regulating drugs should be considered.
Q10. What are the adverse effects of statins?
Although statins are widely used to regulate lipids and prevent cardiovascular accidents, there are still concerns about their safety and prognosis.
Adverse reactions to statins include
Myopathy: an incidence of about 5%, classified as myalgia, myositis, rhabdomyolysis, etc. according to the severity.
Elevated transaminases, with an incidence of 0.5-2.0%, causing liver damage and elevated alanine aminotransferase (ALT) and aspartate aminotransferase (AST).
Adverse effects such as headache and insomnia may also occur.
Q11. How can these adverse effects be mitigated or even avoided?
It is now possible to predict the muscle toxicity and lipid-lowering efficacy of statins by pharmacogenetic testing, thus helping patients to choose the right and good drug, improve the efficacy and reduce the risk of adverse effects.
The SLCO1B1 gene transfers drugs from the blood to the liver for direct efficacy or metabolism to active substances. It has genetic polymorphisms, and the pure mutant type (CC) will result in a reduced ability of the liver to take up drugs, causing an increase in statin blood levels and increasing the risk of myopathy.
The ApoE gene is closely related to the efficacy and prognosis of statins. There are two polymorphisms in the human ApoE gene, forming haplotypes ApoE2, 3, and 4. ApoE4 carriers are at higher risk for coronary heart disease and tend to be less effective on statins, while ApoE2 carriers have the strongest lipid-lowering effect of statins.
It is recommended that SLCO1B1 and ApoE gene polymorphisms be tested in patients who are receiving or considering treatment with statin lipid-lowering drugs. Based on the test results, lipid-lowering efficacy and individual tolerance, the appropriate statin and its optimal drug dose should be selected.
Author: LI JING | Reviewer: LI JING | Editor: LI JING | Source: SAHZU OFFICIAL WECHAT | Date:2021-09-27 | Views:![]()
![]()
![]()
![]()